Abstract
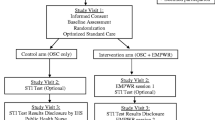
This is a 2-arm pilot randomized controlled trial (N = 96) of a behavioral intervention (4 group and 4 individual sessions) integrating risk reduction counseling with counseling to foster self-acceptance in MSM in India compared to enhanced standard of care (ESOC). Both conditions involved HIV and STI testing and counseling at baseline and 6-months, and assessments of condomless sex at baseline, 3-, and 6-months. A significant condition by time interaction suggested a difference in the rate of change in number of anal sex acts without condoms in the intervention versus ESOC (p < 0.0001). Post hoc contrasts suggested that the overall difference was due to intervention-response at 3-months. The incidence of bacterial STIs was 17.5 % in the intervention condition and a 28.6 % in ESOC. Addressing self-acceptance and related psychosocial concerns in the context sexual risk reduction counseling for MSM in India was feasible and acceptable. Testing the intervention for efficacy is justified.
Resumen
Esto es un estudio piloto de un ensayo clínico aleatorizado (N = 96) que fue proveído en la India con hombres que tienen relaciones sexuales con otros hombres (HSH). El estudio compara una intervención conductual—cual integra consejería para desminuir riesgo con consejería para desarrollar auto-aceptación—con tratamiento estándar y realzado (ESOC en inglés). Ambas condiciones incluyen examen y consejería para el VIH y otras enfermedades transmitidas sexualmente. Estas se llevaron a cabo en las evaluaciones de línea base y de 6 meses, con entrevistas sobre el riesgo sexual completadas durante las evaluaciones de línea base, 3 y 6 meses. Una interacción de condición y tiempo indicaron una diferencia en la tasa de cambio entre la condición conductual comparada con ESOC (p < 0.0001) en la cantidad de actos de sexo anal sin protección. Analices post hoc de contraste indicaron que la diferencia fue a causa de la reacción a la intervención a los 3 meses. La incidencia de enfermedades transmitidas sexualmente fue 17.5 % en la condición conductual y 28.6 % en la condición ESOC. Con este grupo de HSH en la India, se demostró factibilidad y aceptación de poder abordar la auto-aceptación y factores psicosociales como parte de consejería para desminuir el riesgo del VIH. Es justo examinar la intervención para demostrar su efectividad.

Similar content being viewed by others
References
Baral S, Sifakis F, Cleghorn F, Beyrer C. Elevated risk for HIV infection among men who have sex with men in low- and middle-income countries 2000–2006: a systematic review. PLoS Med. 2007;4:e339.
Chakrapani V, Newman PA, Shunmugam M, McLuckie A, Melwin F. Structural violence against Kothi-identified men who have sex with men in Chennai, India: a qualitative investigation. AIDS Educ Prev Off Publ Int Soc AIDS Educ. 2007;19:346–64.
Newman PA, Chakrapani V, Cook C, Shunmugam M, Kakinami L. Correlates of paid sex among men who have sex with men in Chennai, India. Sex Transm Infect. 2008;84:434–8.
Safren SA, Martin C, Menon S, Greer J, Solomon S, Mimiaga MJ, et al. A survey of MSM HIV prevention outreach workers in Chennai, India. AIDS Educ Prev Off Publ Int Soc AIDS Educ. 2006;18:323–32.
Asthana S, Oostvogels R. The social construction of male “homosexuality” in India: implications for HIV transmission and prevention. Soc Sci Med. 1982;2001(52):707–21.
Go VF, Srikrishnan AK, Sivaram S, Murugavel GK, Galai N, Johnson SC, et al. High HIV prevalence and risk behaviors in men who have sex with men in Chennai, India. J Acquir Immune Defic Syndr. 1999;2004(35):314–9.
Gutierrez J-P, McPherson S, Fakoya A, Matheou A, Bertozzi SM. Community-based prevention leads to an increase in condom use and a reduction in sexually transmitted infections (STIs) among men who have sex with men (MSM) and female sex workers (FSW): the Frontiers Prevention Project (FPP) evaluation results. BMC Public Health. 2010;10:497.
Herget G. India: UNAIDS claims law criminalizing homosexuality hinders HIV prevention. HIV AIDS Policy Law. 2006;11:35–6.
Skanland CA. India: Delhi high court annuls law criminalizing adult homosexual relations. HIV AIDS Policy Law Rev. 2009;14:49–51.
Sivasubramanian M, Mimiaga MJ, Mayer KH, Anand VR, Johnson CV, Prabhugate P, et al. Suicidality, clinical depression, and anxiety disorders are highly prevalent in men who have sex with men in Mumbai, India: findings from a community-recruited sample. Psychol Health Med. 2011;16:450–62.
Safren SA, Thomas BE, Mimiaga MJ, Chandrasekaran V, Menon S, Swaminathan S, et al. Depressive symptoms and human immunodeficiency virus risk behavior among men who have sex with men in Chennai, India. Psychol Health Med. 2009;14:705–15.
Mimiaga MJ, Thomas B, Mayer KH, Reisner SL, Menon S, Swaminathan S, et al. Alcohol use and HIV sexual risk among MSM in Chennai, India. Int J STD AIDS. 2011;22:121–5.
Thomas B, Mimiaga MJ, Mayer KH, Johnson CV, Menon S, Chandrasekaran V, et al. HIV prevention interventions in Chennai, India: are men who have sex with men being reached? AIDS Patient Care STDs. 2009;23:981–6.
Mimiaga M, Closson E, Thomas B, Johnson CV, Mayer KH, Bentancourt T, et al. Exploring adverse social conditions and psychosocial health problems among MSM in Chennai, India: a qualitative study. Manuscript under revision.
Meyer IH. Minority stress and mental health in gay men. J Health Soc Behav. 1995;36:38–56.
Stall R, Mills TC, Williamson J, Hart T, Greenwood G, Paul J, et al. Association of co-occurring psychosocial health problems and increased vulnerability to HIV/AIDS among urban men who have sex with men. Am J Public Health. 2003;93:939–42.
Safren SA, Reisner SL, Herrick A, Mimiaga MJ, Stall RD. Mental health and HIV risk in men who have sex with men. J Acquir Immune Defic Syndr. 1999;2010(55 Suppl 2):S74–7.
Thomas B, Mimiaga MJ, Mayer KH, Closson EF, Johnson CV, Menon S, et al. Ensuring it works: a community-based approach to HIV prevention intervention development for men who have sex with men in Chennai, India. AIDS Educ Prev Off Publ Int Soc AIDS Educ. 2012;24:483–99.
Thomas B, Mimiaga MJ, Mayer KH, Perry NS, Swaminathan S, Safren SA. The influence of stigma on HIV risk behavior among men who have sex with men in Chennai, India. AIDS Care. 2012;24:1401–6.
Thomas B, Mimiaga MJ, Kumar S, Swaminathan S, Safren SA, Mayer KH. HIV in Indian MSM: reasons for a concentrated epidemic & strategies for prevention. Indian J Med Res. 2011;134:920–9.
Schaeffer NC, Presser S. The science of asking questions. Annu Rev Sociol. 2003;29:65–88.
Tourangeau R, Yan T. Sensitive questions in surveys. Psychol Bull. 2007;133:859–83.
Rathod SD, Minnis AM, Subbiah K, Krishnan S. ACASI and face-to-face interviews yield inconsistent estimates of domestic violence among women in India: the Samata Health Study 2005–2009. J Interpers Violence. 2011;26:2437–56.
Acknowledgments
Funding from this project is from a joint Indo-U.S. mechanism. Accordingly, Grant NIMH R-21 MH085314 was awarded to Dr. Steven Safren from the National Institute of Mental Health (NIMH) and Dr. Beena Thomas was awarded a Grant from the India Council of Medical Research (ICMR). Dr. Safren was also supported by Grant 5K24MH094214 with respect to investigator time after the R21 funding ended. We would like to thank Jocelyn Remmert for helping prepare the manuscript for submission, and Dr. C. Andres Bedoya for writing the Resumen. We would also like to thank the study participants, and the staff of Sahodaran for their contribution to the project.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Safren, S.A., Thomas, B.E., Mayer, K.H. et al. A Pilot RCT of an Intervention to Reduce HIV Sexual Risk and Increase Self-acceptance Among MSM in Chennai, India. AIDS Behav 18, 1904–1912 (2014). https://doi.org/10.1007/s10461-014-0773-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-014-0773-4