Background and epidemiology: Three years ago it looked as if we were on the brink of eliminating syphilis in Canada. Two decades of data demonstrated a consistent, downward trend in the number of reported cases, with overall rates of infectious syphilis in Canada remaining stable between 1993 and 1996, at about 0.5 per 100 000.1 The only change over this 4-year window was in the age distribution of incident cases. In contrast to previous years, in 1996 syphilis rates were highest among men and women 25–29 years old. At that time it was impossible to draw conclusions from this change; however, the implications have subsequently declared themselves through local resurgence in sexually active populations. The projected overall 2001 rate in Canada rose sharply to 0.9 per 100 000.2 The rate is increasing among both men and women. The most significant change is among men aged 20–24, who experienced a 3.8-fold increase over the past 5 years. Have we dropped the ball? Or have larger social trends made existing control efforts inadequate?

Figure.
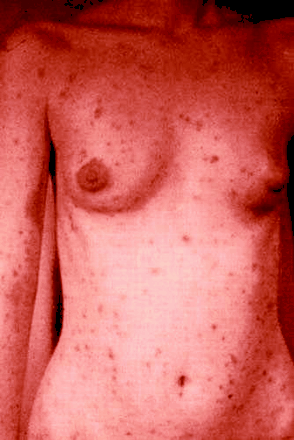
Figure. One-third of untreated patients with syphilis develop a rash Photo by: San Francisco Public Health

Figure. Chancre: the first sign of syphilis, appearing about 3 weeks after infection Photo by: San Francisco Public Health
Syphilis is an STD caused by Treponema pallidum. If untreated, the infection progresses through 5 stages (Table 1). “Infectious” syphilis refers to primary, secondary and early latent stages. Transmission occurs through direct contact with infectious exudates from moist, early lesions of skin and mucous membranes of infected people during sexual contact, nearly always sexual intercourse; transmission is rare after the first year. Infection during pregnancy can lead to miscarriage, stillbirth, premature birth and congenital infection. The incubation period ranges from 10 days to 3 months and is usually 3 weeks. There are important “bidirectional” interactions between syphilis and HIV infection: the presence of genital ulcers, such as those in primary syphilis, increases the risk of HIV transmission 3 to 5 times; the presence of HIV infection may result in atypical presentations of syphilis and may increase the risk of neurological relapse in people with neurological disease.
Table 1.
Clinical management: The primary lesion (chancre) appears about 3 weeks after exposure as an indurated, painless ulcer and may not be clinically evident (i.e., it may be in the rectum or on the cervix). Invasion of the bloodstream precedes the initial lesion. Discovery of a firm, nontender, satellite lymph node is common. After 4–6 weeks the chancre begins to involute. In one-third of untreated cases a secondary eruption occurs: a symmetrical maculopapular rash involving the palms and soles that is accompanied by constitutional signs. This eruption, which can also affect other parts of the body, usually resolves spontaneously within weeks to months, but it may recur. About one-third of untreated cases become clinically latent for weeks to years. Syphilitic meningitis may occur anytime within secondary or early latent stages. Unpredictably, up to 2 decades after initial infection, disabling lesions, caused by obliterative small-vessel endarteritis, appear in the aorta, or gummas (granulomatous lesions) occur in the skin, central nervous system (CNS), viscera, bone or mucosal surfaces. Neurosyphilis must be considered in the differential diagnosis of HIV-positive people with CNS symptoms.3
Diagnosis is made by dark-field microscopy of genital ulcers in primary syphilis and by serologic testing in all later stages. Two forms of serologic testing are available: nontreponemal antigen tests (e.g., VDRL [Venereal Disease Research Laboratory] or RPR [rapid plasma reagin]), which are used for screening specimens, and treponemal antigen tests (e.g., MHA-TP [microhemagglutination assay–T. pallidum] or FTA-ABS [fluorescent treponemal antibody absorption]), which are used for confirmation of nontreponemal antigen test results. Although nontreponemal antigen tests are less sensitive and less specific than treponemal antigen tests, they are preferred for screening because of their low cost. A polymerase chain reaction assay for T. pallidum exists, but it is not widely available in clinical settings.
Treatment is usually with penicillin: long-acting benzathine penicillin G (2,4 million U intramuscularly) as a single dose for primary, secondary or early latent syphilis and as 3 weekly doses for late latent or tertiary syphilis. An alternative therapy for nonpregnant patients allergic to penicillin is either doxycycline (100 mg orally twice daily) or tetracycline (500 mg orally 4 times daily) for 14 days in people with primary, secondary or early latent syphilis or for 28 days in people with late latent or tertiary syphilis. Neurosyphilis is usually treated with high-dose intravenous penicillin or intramuscular procaine penicillin therapy with probenecid for 10–14 days. Follow-up serologic testing after treatment should be carried out until an adequate response is achieved. Recent difficulties with the supply of benzathine penicillin in Canada may complicate the management of syphilis, but benzathine penicillin should be obtainable in most Canadian jurisdictions with the assistance of local public health authorities. A recently published pilot study suggested that azithromycin as a single 2-g oral dose may be equivalent to penicillin for the treatment of primary, secondary or early latent disease.4
Prevention: The correct and consistent use of condoms can reduce the risk of transmission. Serologic testing for syphilis should be included in the work-up of all STD cases and as a routine part of prenatal examinations. All cases must be reported to the public health department for investigation of contacts and the source of infection. The use of public advertising to increase awareness of signs and symptoms of syphilis may be helpful, although it may cause local controversy. The stage of disease determines the criteria for partner identification. Cases and contacts should also be counselled about the need for HIV testing.5
Erica Weir CMAJ David Fishman Associate Medical Officer of Health Hamilton, Ont.










